Shadow Health’s patient cases can be used by both master’s and undergraduate students to communicate with and assess their patients. An Advanced Shadow Health Assessment patient research refers to the evolution of Tina Jones’ single-framework valuations after regular visits to the health institution over the course of a simulated year, which scholars have found useful in planning for their medical assessment.
Furthermore, this case study allows learners to record their research, which aids in blending the data collected when communicating with their patients.
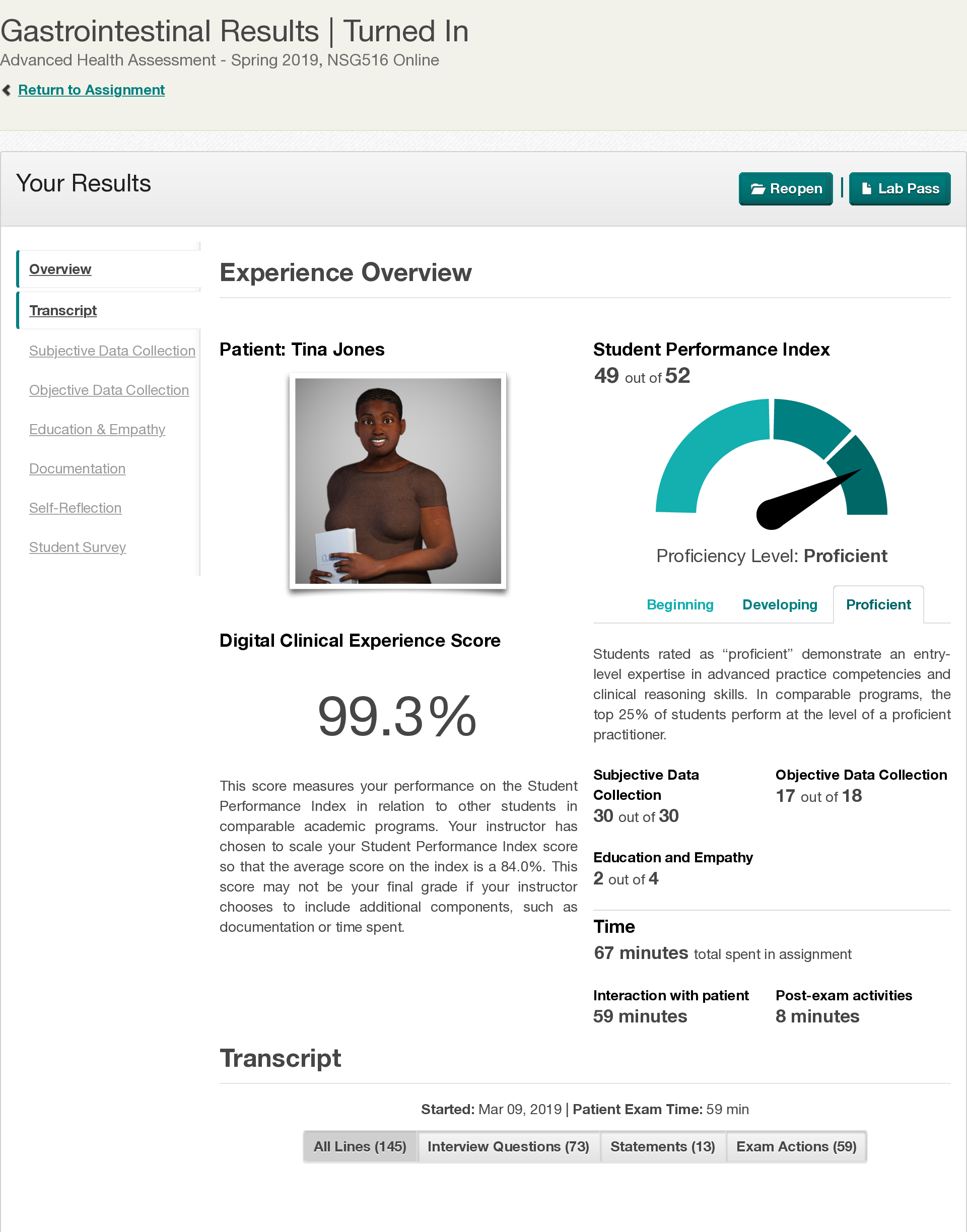
Tina Jones Respiratory Shadow Health Assessment
Tina had had an asthma attack two days before.
During this time, she relied on her albuterol inhaler to treat her asthma; even when the symptoms subsided, the inhaler was never used to treat the condition.
Tina noticed she had ten wheezing attacks and was frequently winded since the asthma attack. To conduct an accurate patient assessment, you must answer pertinent questions about the symptoms you are experiencing with your body.
This study will aid in the assessment of any lung sounds during the actual medical evaluation.
When writing a Shadow Health Assignment, you will analyze the collected data using appropriate medical terminology.
Tina Jones Comprehensive Assessment Shadow Health
Tina Jones, a 28-year-old African-American woman, came to our clinic complaining of breathing difficulties and windedness following asthma attacks. Tina claims she went to see her cousin and came across several kittens, which is where her asthma symptoms began. She noticed her wheezing rate was 6/10 and her windedness was 8/10, both of which lasted at least five minutes. Tina, according to her assessment, never experienced any chest pains or hypersensitive side effects. During this time, she dealt with asthma attacks by using her albuterol inhaler, which only helped her manage some symptoms. Ms. Jones discovered that she had ten wheezing episodes and was frequently winded after her asthma attack. She had windedness symptoms at home prior to visiting the health center. Ms. Jones notices that some of her systems are compromised after lying down at a certain angle, which is accompanied by painful coughs. You must include the above information when completing a Shadow Health Respiratory Physical Assessment Research.
Tina gets winded about twice a night while sleeping. Ms. Jones claims that her symptoms are interfering with her daily activities and that her albuterol inhaler may no longer be as effective as it once was. She claims that her breathing has improved since further diagnosis. Ms. Jones was diagnosed with asthma when she was two years old. She has never smoked, has never used a pinnacle stream, has no medical history of pain, and does not own a home vaporizer. According to the medical evaluation of Ms. Jones, she was last hospitalized for asthma at the age of 16 and has never been intubated for her asthma. For a complete assignment on any Shadow Health Case Study, the instructor expects students to include the above information.
Tina jones cardiovascular shadow health
- Consulted regarding any heart problems:
– Disagrees regarding any heart complications
- Heartbeat rates were discussed:
– Accounts for a normal heartbeat
– Reports a regular pulse – Disavows palpitations
– Refuses to acknowledge arrhythmia
- Hypertension was discussed.
– Hypertension disagreements
– Reports her most recent circulatory strain following her diagnosis:
– Reports that the last pulse was 140, rather than 80 or 90.
– Accounts for a belief that her current pulse is on the high side of normal range.
- When asked about the heart mumble,
– Any heartfelt disagreements are mumbled.
- When asked about swelling,
– Apart from having a foot wound, he disagrees on any swelling.
- consulted about any blue skin signs
– blue skin disagrees
- I was asked if I wanted to have a heart analysis.
– Disagrees on seeing a psychiatrist – Disagrees on any echocardiogram signs
– No coronary artery CT X-ray diagnosis was performed
- Consulted about any heart medical procedures – No heart surgeries were performed – Disagrees about angioplasty or stent – Disagrees about having a pacemaker
- When asked if he had any chest problems,
– Disagrees on the possibility of experiencing any chest complications
– Disagreements about having angina
- In case of a heart attack or chest tightness, consult a doctor.
– Claims to have had chest tightness while being treated for asthma
– Does not report having had chest tightness recently
Tina Jones Neurological Shadow Health
- Concerning the strike, the following information was requested:
– There is no medical history of having had a stroke.
– Disagrees on any recent numbness symptoms
- When confronted with quivering:
– Disagrees about shivering
- If you have any vision problems, please consult with the following people:
– Makes claims about having vision problems
– The importance of having vision problems was emphasized.
– Following further evaluation, she claims to have had vision problems in recent months. Tina claims to have foggy vision regularly
– She claims to have reading vision problems but denies having double eyesight.
- Consulted about migraines:
– Allegations of sporadic cerebral pains
– Describes the cerebral pain that has occurred in the last few days.
– Disagrees on having recently suffered from migraines
- When asked if he had any cerebral pain, he said no.
– Ms. Jones claims to have regular cerebral pains
– claims to have had migraines in the last few hours
– claims to have had cerebral pains several times a month
- When asked about cerebral pain triggers, Ms. Jones says she gets them whenever she anticipates something.
- When asked if they have any symptoms of cerebral pain
– Tina claims that her migraines aren’t life-threatening
– She reports having cerebral pains on the sides of her head; she claims to have tight migraines; and she says the cerebral pains have been bothersome.
- When asked if she had ever received migraine treatment, she stated that she had once used acetaminophen to treat cerebral pains.
– She stated that she had used regular-strength acetaminophen medicine.
– When asked if she had ever experienced dizziness, she stated that she had never experienced it.
Tina Jones Musculoskeletal Shadow Health
- Any joint issues were discussed.
– Obtained information about her joint pains
– Obtained reports on joint swelling
- questioned about adaptability
– Identifies a history of walking difficulties
– Tina claims to have had a wound that caused her walking difficulties.
- Questioned about whether she felt pain while moving
– claims to feel more pain when walking Consulted about her ability to stand
– Before she was injured, I gathered information about her position.
- When asked if he had any muscle pains, he said no. gathered pertinent information about her history of muscle pains
– I also gathered information about her recent muscle pain.
- When asked if the injury had impacted her work, she stated that it had not.
– Is your job hazardous?
– Do you move around a lot at work?
– What is it that keeps you from doing well at work?
- Consulted about ADLs
– Can you move from a sitting to a standing position?
– Do you encounter any difficulties while taking a bath?
Tina Jones Abdominal Assessment
- When asked about distinguishing bowel characteristics,
– Do you have bowel movements regularly?
-When was the last time you had a bowel movement?
- Consulted for constipation -Have you recently been constipated? Have you experienced hard stools?
– Do you have any difficulties with bowel movements?
- Screening was performed on the stool sample.
-What is the stool’s shape?
-Can you tell me what color the stool is?
-Is there blood in the stool?
- When asked about gassiness, she wondered if there was any bloating.
Shadow Health Tina Jones Health History
A good research paper on Tina Jones’s history should include questions about Tina’s current and past health, from her recent foot wound to any pre-existing disorders. Ms. Jones’s body parts should also be evaluated, as well as her psychosocial history and family health records. This evaluation will assist you in creating detailed health records for Tina Jones. If you discover any illnesses, inquire about the symptoms and how the patient dealt with the diseases as they arose.
During the assessment, you will need to educate and empathize with Ms. Jones to develop her sense of well-being. Tina’s comprehensive medical history will require you to ask her pertinent questions. When communicating with the patient in available and formal language, you will need to use medical phrases to obtain accurate information with the assistance of medical recordings, discoveries, and nursing articles. Following completion of the evaluation activities, you will need to go over the findings step by step. You will be required to perform data handling activities to obtain Ms. Jones’ medical history. Finally, you will identify and discuss the evaluation before developing a structured approach to the problematic assessment.
Shadow Health Tina Jones Questions/Answers
1. What criteria will the instructor use to evaluate my work?
The instructor will grade your research based on your knowledge of the subject matter, as well as your Education and Understanding. To complete and achieve your Education and Empathy, you must respond to the condition that requires restorative communication as soon as possible. When communicating with your patient, you will think about the format of your questions, which can be therapeutic or definitive. Furthermore, this can be accomplished by conducting extensive and in-depth research on the patient’s health. When handling your research, your instructor will also evaluate your ability to collect data and how you structure your nursing research. It may take 90-110 minutes to gather relevant information for the assessment. As it is a safe restoration, completing the given assignment may take longer than expected; however, every student can have ample time to develop and discover their abilities.
2. How will this assignment help me prepare for the real world?
After completing this assignment, you will have acquired skills and information about the structure and content of health history assessments on your patients; as a medical professional, you will be able to:
- Create appropriate and well-structured questions
- Gather information about your patient’s medical history.
- Consider the risks that your patient may face as a result of the disorder or illness.
- Replicate what you know and identify areas where you need to improve.
- Identify and have detailed information about the nursing assessment.
- Concentrate on creating a well-structured nursing assessment.
3. What else would you add to this assignment?
To ensure your patient’s health, well-being, and safety, you must answer your nursing questions. You can use the Electronic Health Record as a health practitioner to create a report of your patient’s results. The healthcare practitioners will have relevant information about their patients if these results are recorded. Aside from subject information collection, healthcare professionals can engage in other renovation activities that provide them with pertinent information about their patients.
To assess Tina’s spinal levels l2, l3, and l4, which deep tendon reflexes would have to be tested?
A patellar profound ligament reflex should have solid and functional nerve strands in the L2, L3, and L4 spinal ranks. The study of rare reflexes aids in distinguishing neurological pathologies of the spine.
Tina Jones Heat
Finding: The main complaint was established.
Tina claims to have a sore throat (Results) Pro Tip: Any protest against a patient will aid in the discovery of any disorder. Achieving any of the outcomes of the demonstration will assist the patient in communicating any emerging side effects.
Example Question: Does your throat itch?
Ms. Jones claims to have had a scratchy throat (Outcomes) Professional Guidance: The main goal of setting up a protest on your patient is to discover any arising disorder. This protest will encourage the patient to discuss any side effects of the disease.
Example Question: Does your throat itch?
Ms. Jones claims to have itchiness in her eyes as a result of the results (Results) Pro Tip: Performing a protest on your patient will aid in the analysis of any illness or symptoms that may arise. This allows the patient to speak freely about any signs and symptoms.
Example Question: Are your eyes itchy?
Ms. Jones reports having a runny nose after a few consultations (Outcomes) Recommendation from a Professional: Performing a protest on your patient will aid in the analysis of any illness or symptoms that may arise. The practitioner will be able to communicate with their patients and open up about any symptoms if they are aware of any disorders.
Example Question: Do you have a runny nose?
History of Present Illness
Finding: Consulted about the disorder’s current signs and symptoms.
Ms. Jones claims that the sore throat began within the last week (Outcomes) Professional Guidance: Inquiring with your patient about the duration of their most recent illness will help you learn more about the history of their current disorder. Having this data will assist you in detecting any current diseases or symptoms, analyze the area of their pain, or measure the pain she may be experiencing.
Question Example: How long have you had a sore throat?
Ms. Jones claims that the runny nose started a week ago (Results) Professional Guidance: Inquiring with patients about how long they have been suffering from the current disease provides information about their illness’s history. Gathering information about the current condition will assist you in reevaluating the signs and symptoms of the current disease, such as measuring the pain they may be experiencing.
Question Example: When did your nose start running?
Ms. Jones reports that the itching in her eyes began a week ago (Outcomes) Professional Guidance: Inquiring with patients about how long they have been suffering from the current disease provides information about their illness’s history. Gathering information about the current condition will assist you in reevaluating the signs and symptoms of the current disease, such as measuring the pain they may be experiencing.
Question Example: When was the last time your eyes itched?
Findings: Consulted about the leading causes of throat symptoms.
Ms. Jones claims to be suffering from chronic throat pains (Outcomes). Professional Guidance: Collecting information about the time she has been afflicted with the current health disorder will assist you in obtaining relevant information about the current disease. Conducting a current protest allows you to reevaluate the disease’s recent signs and symptoms.
Example Question: Is it common for you to have throat pain regularly?
Ms. Jones claims that her throat pain worsens in the morning (Results) Professional Advice: Gathering information about the patient’s time suffering from the current disorder aids in reanalyzing the past signs and symptoms of the current illness.
Example Question: When does your sore throat get worse?
Tina claims to have sore throat when she swallows (Outcomes) Professional Guidance: Gathering information about Ms. Jones’s recent illness aids in obtaining relevant information about the history of the current disease. Collecting information about the length of time the patient has been afflicted with the current disorder aids in reanalyzing the past signs and symptoms of the current illness.
Question Example: How often does it hurt to swallow?
PLACE THIS ORDER OR A SIMILAR ORDER WITH NURSING PAPERS MARKET TODAY AND GET AN AMAZING DISCOUNT
